Scoliosis – a Prevalent, Yet Unrecognized Condition Plaguing Many Adults
Scoliosis is often thought of as a condition that only affects teenagers, however, scoliosis in adults is common, progressive and typically incorrectly diagnosed.
While it is true, the rate of scoliosis in adolescents, particularly the idiopathic type, is relatively high (0.47% – 5.2%)[1], scoliosis can actually develop at any time. In fact, contrary to popular belief, scoliosis is highly prevalent in adult populations, with estimates as high as 68% reported in patients aged 60-90 years[2]. It is also believed that this will increase over the next 20 years as people continue to live longer life spans.
Adult scoliosis can have a variety of causes. The most common types are adult degenerative scoliosis (De Novo Scoliosis) and pre-existing idiopathic scoliosis.
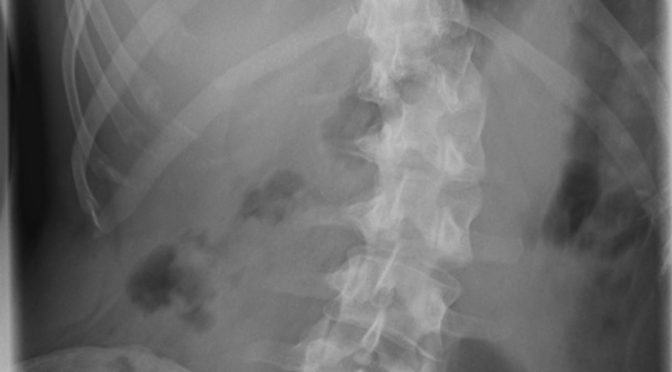
x-ray of an adult with scoliosis
Adult degenerative scoliosis is often the result of newly developed asymmetrical disc degeneration or injury, usually in the lumbar or thoracolumbar spine. The loss of disc height creates asymmetrical loading which can set up a cycle of continued degeneration and often results in pain.
For other adults, their scoliosis is a continued progression of one of the idiopathic forms of scoliosis (infantile, juvenile or adolescent) into adulthood. They may not have received proper treatment in their younger years and their symptoms have become more severe as their curve naturally advanced over the years.
While it can sometimes be difficult to differentiate between the various types of adult scoliosis, most patients will present with back pain accompanied by a worsening posture, often a forward hunch, and they report an impact on their quality of life. In the more severe cases, patients may experience leg pain, spinal cord compromise and/or walking difficulty.
No matter the situation from adolescence to adulthood, early detection of scoliosis is paramount to the outcomes. No matter the case, getting appropriate corrective care will have an impact.
Key indicators for adult scoliosis can include:
- A family history of scoliosis
- Uneven shoulder heights or waist curves
- Rib humping when bending forwards
- Significant loss of standing or sitting height
- Postural changes/collapse
These can co-exist with other clinical factors such as history of surgery, menopause or a diagnosis of osteopenia/osteoporosis, all of which can have a compounding effect on scoliosis progression.
Early detection and accurate diagnosis, combined with early scoliosis treatment will lead to better clinical outcomes and quality of life.
If you or someone you know has noticed a change in posture, are in pain, or have a family history of scoliosis, please schedule a free screening today.
To schedule, a free case review click here or call 970-207-4463.
References
- Konieczny MR, Senyurt R, Krauspe R. Epidemiology of adolescent idiopathic scoliosis. J Child Ortho, 2013. 7(1): p. 3-9.
- Schwab F, et al. Adult scoliosis: prevalence, SF-36, and nutritional parameters in an elderly volunteer population. Spine, 2005. 30(9): p. 1082-5.
